What is the Treatment for Varicose Veins?
- What are varicose veins?
- How are varicose veins different from spider veins?
- What causes varicose veins?
- How do you treat varicose veins?
- Can you prevent varicose veins?
The blue, red, and purple veins can pop out in your legs almost overnight. If this happens to you, don’t be alarmed; varicose veins are actually quite common. In fact, 23% of Americans suffer from a circulatory problem called varicose veins. That’s about 20 to 25 million people.
Varicose veins signal a disruption in the body’s circulatory system. Both superficial and deeper veins can malfunction, causing the unsightly roadmap sometimes visible through the skin that you may be familiar with. Thin, less visible veins can also appear, and these are known as spider veins. Either condition can be noticeable but only varicose veins can cause discomfort, swelling and restless legs.
At Coastal Vascular & Interventional, PLLC, we treat varicose veins and spider veins, which are not entirely the same thing but they can be caused by the same problem: venous insufficiency.
Let’s take a closer look at varicose veins, how they differ from spider veins, and how you can prevent and treat this condition.
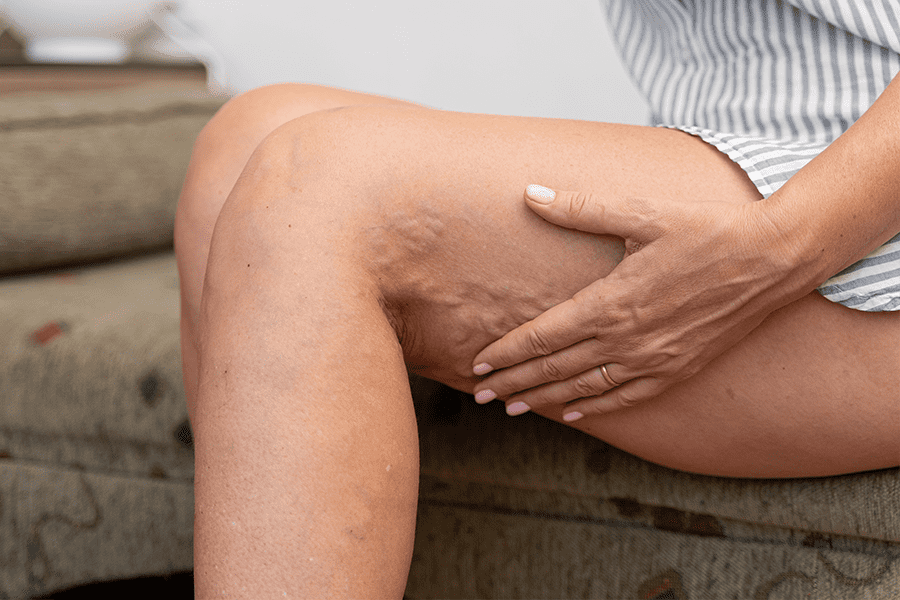
What Are Varicose Veins?
Varicose veins are enlarged, twisted veins that occur under the skin. Veins that are close to the skin surface can also be affected. Varicose veins often occur in the legs.
When varicose veins first appear, you may not notice other adverse symptoms. However, varicose veins can also become quite uncomfortable over time. A lot of times, the reflux in the veins can cause the feeling of heaviness, fatigue, cramping or achiness. Extensive edema or swelling in the legs from varicose veins can also cause open non healing wounds, or injuries to legs not to heal. These are the symptoms that often compel patients to have their legs looked at by a medical professional.
It’s also important to note that you can have varicose veins or venous reflux without physically seeing the veins.
If you have symptoms stemming from your varicose veins, you could experience:
- Aching in the limbs
- Ankle and/or leg swelling
- Burning and pain around the varicose vein
- Itching around the area
- Non-healing wounds
- Tension and restlessness in the affected extremity
Varicose veins are often lumped together with a milder form of circulatory issue called spider veins. What’s the difference between spider and varicose veins?
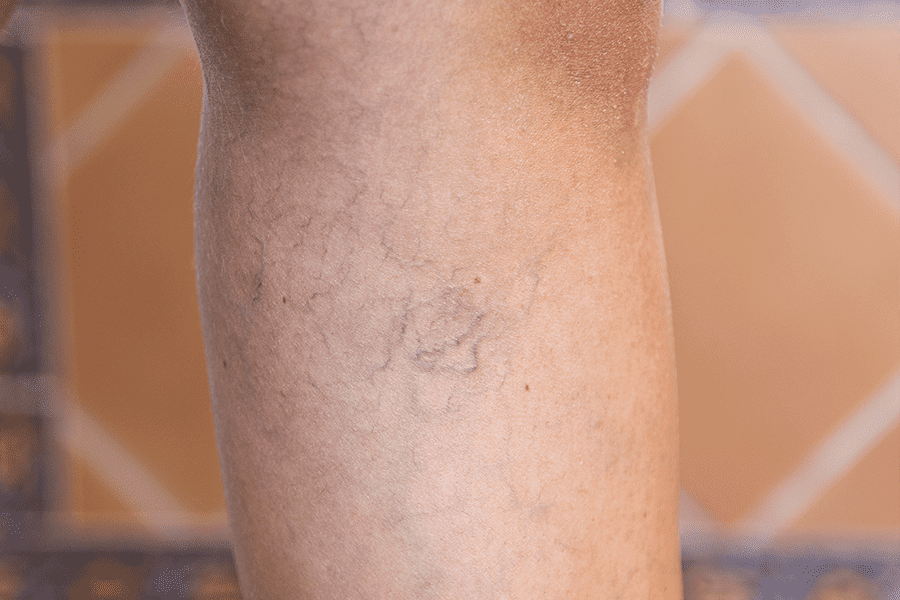
How Are Varicose Veins Different from Spider Veins?
The biggest difference between varicose veins and spider veins is their size. Varicose veins are larger, swollen, and painful, crisscrossing the skin as mounds of red, blue, and purple. Spider veins may be the same color, but they are more sedate, appearing just under the skin as a line, and not a hill. Spider veins can form anywhere, but we see them most often on the legs, face and chest.
Spider veins can be a sign of an underlying condition from varicose veins, but that’s not inevitable by any means. Varicose veins can become problematic, causing several complications. This includes:
- Skin ulcers/non healing wounds that form over the varicose veins
- Blood clots
- Bleeding from a ruptured vein
Given that these symptoms can be quite serious, it’s important to understand what causes varicose veins and what you can do to prevent them.
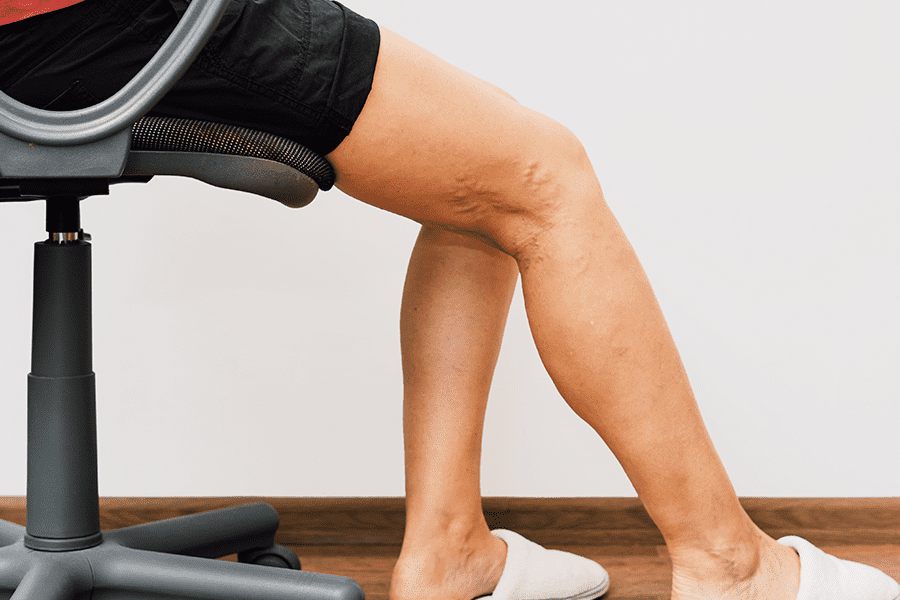
What Causes Varicose Veins?
Varicose veins stem from damaged or weak valves within your veins. The body’s circulatory system is made up of a series of veins and arteries that bring blood across the body from the heart. Arteries are the lines that bring blood pumped from the heart out to the extremities. Then the veins return that blood back to the heart. To do this, the veins must fight gravity to reach their destination.
Inside your legs, tiny muscle contractions pump the blood back toward the heart. Inside the veins, there are tiny valves that open to allow the blood to flow through toward your heart. When these valves become damaged, the blood begins pooling in the veins and causing them to twist, stretch, and bulge. On the surface of the skin you experience a varicose vein, a visible indicator that the vein isn’t working correctly.
At Coastal Vascular & Interventional, PLLC, patients will sometimes come in and say “My legs swell and ache, but have no visible varicose veins’’ Sometimes varicose veins can be caused from prolonged standing or from genetics.

How Do You Treat Varicose Veins?
When it comes to treating varicose veins, our vascular surgeons have minimally invasive treatments to treat varicose veins. The most common procedures for treating varicose veins include:
- Radiofrequency ablation (RFA)
- Endovenous Laser Ablation Therapy (EVLT)
- VenaSeal, which a procedure that uses an adhesive to close up the offending vein
- Foam sclerotherapy
Other recommendations for treating this condition and its symptoms include:
- Compression stockings to help with swelling
- Injection therapy, or sclerotherapy, that places a solution in the vein to irritate the inside of the vein and cause it to collapse.
- Leg elevation to decrease the pressure on your veins
- Nsaids or anti inflammatory medications
Additionally, while these are the most common treatments for varicose veins, you may be able to prevent them from occurring with a few lifestyle changes.
Can You Prevent Varicose Veins?
A variety of factors can contribute to varicose veins. Genetics can play a role in it. Aging and family history can make you more susceptible to developing varicose veins, and that isn’t something you can do much about.
Some important advice we often give our patients is to get up and walk around every 20 minutes, and if you’re standing, try and move around frequently. Sitting in the same spot for three or four hours contributes to distending your veins and may cause the valves to stretch out and damage.
One option for prevention that we recommend is to wear compression socks. Even if you don’t have a family history and you do a lot of standing or sitting, compression socks provide that external support that prevents varicose veins and spider veins from forming over time.
If you’re struggling with this condition, you can schedule a consultation by contacting our team online or giving us a call at 1-850-479-4223.